Ivermectin’s Anti-Cancer Mechanisms: From Autophagy to Tumor Microenvironment
Ivermectin is an FDA-approved macrocyclic lactone antiparasitic that has been used safely by over 200 million people annually in the treatment of parasitic infections including onchocerciasis (river blindness) and lymphatic filariasis. In recent years, a growing body of preclinical research has examined whether its molecular targets — many of which are expressed in human cancer cells — may confer anticancer activity across multiple malignancy types.
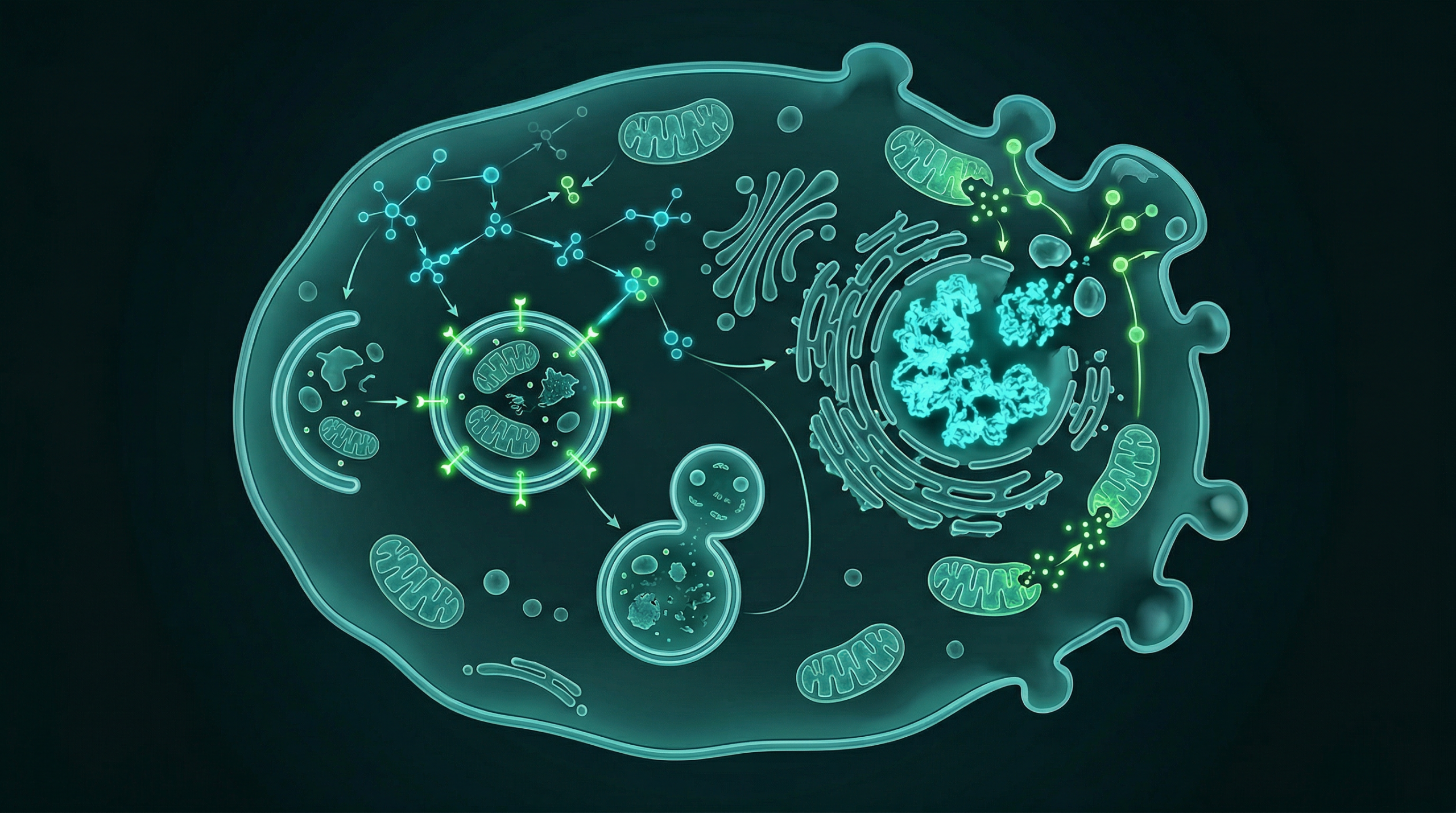
Unlike single-target chemotherapy agents, ivermectin appears to interact with several distinct biological pathways simultaneously. Laboratory studies have identified mechanisms including inhibition of the Wnt/β-catenin signaling axis, disruption of mitochondrial function, blockade of the PAK1/Akt/mTOR pathway, modulation of purinergic receptors, induction of autophagy and apoptosis, and interference with multidrug resistance transporters. The breadth of these mechanisms has prompted researchers to classify ivermectin as a multi-targeted cancer drug candidate.
Wnt/β-Catenin Pathway Inhibition
The Wnt/TCF signaling pathway is frequently activated in colorectal, breast, and other cancers, driving proliferation, survival, and stem cell renewal. A 2014 study by Melotti et al. published in EMBO Molecular Medicine was among the first to document that ivermectin and related macrocyclic lactones inhibit WNT-TCF target gene expression in human cancer cells. The study found that ivermectin mimics dominant-negative TCF activity, represses C-terminal β-catenin phosphoforms, and suppresses CYCLIN D1 — a key proliferative effector of the Wnt pathway.
Critically, in vivo experiments in this study demonstrated that ivermectin selectively inhibited TCF-dependent xenograft tumor growth in mice without producing observable side effects. This selectivity for Wnt-active tumors has implications for patient stratification in any future clinical application.
A subsequent study by Li et al. (2022) extended these findings to demonstrate that ivermectin inhibits tumor metastasis via the Wnt/β-catenin/integrin β1/FAK signaling axis in colorectal and breast cancer cell lines, suppressing migration-related proteins and reducing xenograft metastases. This anti-metastatic dimension adds a second layer of potential clinical relevance beyond primary tumor suppression.
PAK1/Akt/mTOR Axis and Autophagy Induction
PAK1 (p21-activated kinase 1) is overexpressed in approximately 30% of breast tumors and plays a central role in Akt-mediated survival signaling. A 2016 study by Dou et al. in Cancer Research demonstrated that ivermectin induces cytostatic autophagy in breast cancer cells by promoting ubiquitination-mediated degradation of PAK1, which in turn reduces Akt phosphorylation and blocks downstream Akt/mTOR signaling.
The distinction between cytostatic autophagy (which arrests tumor growth) and cytotoxic autophagy (which kills cells) is important: the Dou study found that ivermectin-induced autophagy primarily inhibited tumor growth rather than directly killing cells via autophagic death, though subsequent apoptotic activation was also observed. In xenograft models, ivermectin suppressed tumor growth through this PAK1-mediated pathway.
A parallel study by Wang et al. (2020) confirmed the same PAK1 mechanism in oesophageal squamous cell carcinoma, suggesting this pathway is broadly operative across ivermectin-sensitive cancer types and not specific to breast cancer cell lines.
- Wnt/TCF inhibition: Ivermectin represses β-catenin/TCF signaling and suppresses CYCLIN D1, inhibiting TCF-dependent xenograft tumor growth in vivo without observable toxicity.
- PAK1-mediated autophagy: Ivermectin induces cytostatic autophagy by degrading PAK1 and blocking the Akt/mTOR survival axis in breast cancer and other cancer types.
- Immunogenic cell death: Via P2X4/P2X7 purinergic receptor modulation, ivermectin triggers caspase-1-dependent pyroptosis with ATP and HMGB1 release — hallmarks of immunogenic tumor killing.
- MDR pump inhibition: Ivermectin inhibits P-glycoprotein (MDR1) and ABCG2/BCRP transporters, potentially restoring chemosensitivity in drug-resistant cancer cells.
- Clinically feasible concentrations: Antitumor effects across 28 cancer cell lines were observed at 5 µM — a concentration achievable based on published human pharmacokinetic data.
- Synergy with chemotherapy: Ivermectin demonstrated synergistic activity with docetaxel, cyclophosphamide, and tamoxifen in breast cancer models at clinically relevant concentrations.
Purinergic Receptor Modulation and Immunogenic Cell Death
A less commonly discussed but mechanistically important target of ivermectin is the P2X4/P2X7 purinergic receptor axis. A 2015 study by Draganov et al. in Scientific Reports demonstrated that ivermectin allosterically modulates P2X4 receptors on breast cancer cells, switching purinergic signaling from a pro-survival mode to a cytotoxic mode. This results in caspase-1-dependent pyroptosis — a form of programmed inflammatory cell death distinct from classical apoptosis.
The biological significance of pyroptosis in cancer extends beyond simple cell killing. The process involves release of ATP and HMGB1, which are damage-associated molecular patterns (DAMPs) that signal immune cells, potentially converting an immunologically “cold” tumor microenvironment into an “inflamed” one. This immunogenic cell death (ICD) dimension suggests ivermectin may interact with anti-tumor immune responses, a hypothesis that warrants further investigation in immunocompetent models.
Mitochondrial Dysfunction and Chloride Channel Activation
Ivermectin functions as an activator of glutamate-gated chloride channels, causing ionic imbalance in affected cells. In cancer cells, this disruption appears to translate into mitochondrial dysfunction, including altered mitochondrial membrane potential and increased reactive oxygen species (ROS) production. A comprehensive 2020 mechanism review by Liu et al. in Drug Design, Development and Therapy described this pathway in detail, noting that ivermectin-induced mitochondrial dysfunction operates in parallel to — and may synergize with — its effects on PAK1/Akt and Wnt/TCF pathways.
The convergence of multiple death-inducing signals from these pathways may help explain why ivermectin shows cytotoxic activity at concentrations achievable in clinical settings, whereas compounds relying on a single mechanism often require suprapharmacological concentrations to achieve equivalent effects in vitro.
| Pathway / Target | Effect in Cancer Cells | Key Reference |
|---|---|---|
| Wnt/β-catenin / TCF | Inhibits TCF target genes; represses CYCLIN D1; blocks xenograft growth | Melotti et al., EMBO Mol Med 2014 |
| PAK1 / Akt / mTOR | Cytostatic autophagy via PAK1 degradation; reduced Akt phosphorylation | Dou et al., Cancer Res 2016 |
| P2X4 / P2X7 purinergic receptors | Pyroptosis (caspase-1); ATP/HMGB1 release; immunogenic cell death | Draganov et al., Sci Rep 2015 |
| Chloride channels / mitochondria | Ionic imbalance; mitochondrial dysfunction; increased ROS | Liu et al., Drug Des Devel Ther 2020 |
| SIN3A/B (epigenetic) | Selective inhibition of SIN3 co-repressor complex at clinically achievable concentrations | Juarez et al., Am J Cancer Res 2018 |
| MDR1 / ABCG2 (P-gp / BCRP) | Inhibits drug efflux transporters; may restore chemosensitivity in MDR cancer cells | Pouliot et al., Biochem Pharmacol 1997 |
Epigenetic Targeting via SIN3 Complex
Ivermectin and related avermectins have been shown to selectively inhibit the SIN3 transcriptional co-repressor complex (including SIN3A and SIN3B) at concentrations achievable in clinical pharmacokinetic studies. The SIN3 complex regulates histone deacetylation and chromatin remodeling, and its dysregulation is implicated in several cancer subtypes, particularly triple-negative breast cancer. This epigenetic dimension adds a further layer to ivermectin’s multi-target anticancer profile that is mechanistically distinct from its antiparasitic activity.
Multidrug Resistance Inhibition
P-glycoprotein (MDR1/ABCB1) and BCRP (ABCG2) are ATP-binding cassette (ABC) transporters that actively export chemotherapy drugs out of cancer cells, representing a dominant clinical mechanism of acquired drug resistance. A foundational 1997 study by Pouliot et al. in Biochemical Pharmacology demonstrated that ivermectin reverses P-glycoprotein-associated multidrug resistance in cancer cells. More recent work has characterized ivermectin as a pan-inhibitor of ABC transporters including ABCG2/BCRP, with an IC50 of approximately 23.4 µM.
This MDR-inhibitory activity is particularly notable because it suggests ivermectin may function as a chemosensitizer — restoring the efficacy of conventional chemotherapy in cells that have become resistant through transporter upregulation. This application would not require ivermectin to function as a standalone cytotoxic agent but rather as a pharmacological adjunct.
Activity at Clinically Feasible Concentrations
A key practical question in drug repurposing is whether the concentrations required for in vitro activity can be achieved in human patients through standard dosing. A 2020 study by Juarez et al. in Cancer Chemotherapy and Pharmacology directly addressed this by testing ivermectin at 5 µM — a concentration supported by published human pharmacokinetic data — across 28 malignant cell lines. Antitumor effects were observed across the panel, with breast cancer lines (MDA-MB-231, MDA-MB-468, MCF-7) and ovarian cancer line SKOV-3 showing the greatest sensitivity.
In the same study, ivermectin demonstrated synergistic activity with docetaxel, cyclophosphamide, and tamoxifen, and reduced tumor size and weight in tumor-bearing mice. Cancer stem cell-enriched populations showed reduced viability compared to parental cell lines, suggesting ivermectin may have activity against chemotherapy-resistant stem cell compartments that drive tumor recurrence.
A comprehensive 2018 review by Juarez et al. in American Journal of Cancer Research synthesized the full mechanistic picture, confirming that ivermectin’s anticancer targets — MDR protein, Akt/mTOR, WNT-TCF, purinergic receptors, PAK1, SIN3A/B, RNA helicase, and chloride channels — are all engaged at concentrations that appear achievable based on clinical pharmacokinetic modeling.
The research described in this article is based on preclinical in vitro and in vivo studies. Ivermectin is not approved as a cancer treatment by any regulatory authority, and its use outside of approved antiparasitic indications has not been validated in clinical trials for oncology. This article does not constitute medical advice. Patients with cancer should consult their oncologist for evidence-based treatment guidance.
Summary
Preclinical evidence suggests that ivermectin engages multiple anticancer mechanisms at pharmacologically relevant concentrations: Wnt/β-catenin and PAK1/Akt/mTOR pathway inhibition, immunogenic cell death via purinergic receptor modulation, mitochondrial dysfunction, epigenetic SIN3 complex targeting, and MDR transporter inhibition. These mechanisms act across diverse tumor types and have been validated in both cell culture and animal models.
The breadth of ivermectin’s molecular targets, combined with its well-characterized safety profile from decades of antiparasitic use, makes it a compound of significant interest for formal oncology drug development. Human clinical trials would be necessary to determine whether preclinical efficacy signals translate to clinical benefit.
- Melotti A, Mas C, Kuciak M, et al. The river blindness drug Ivermectin and related macrocyclic lactones inhibit WNT-TCF pathway responses in human cancer. EMBO Mol Med. 2014;6(10):1263-1278. PubMed
- Dou Q, Chen HN, Wang K, et al. Ivermectin Induces Cytostatic Autophagy by Blocking the PAK1/Akt Axis in Breast Cancer. Cancer Res. 2016;76(15):4457-4469. PubMed
- Draganov D, Gopalakrishna-Pillai S, Chen YR, et al. Modulation of P2X4/P2X7/Pannexin-1 sensitivity to extracellular ATP via Ivermectin induces a non-apoptotic and inflammatory form of cancer cell death. Sci Rep. 2015;5:16222. PubMed
- Juarez M, Schcolnik-Cabrera A, Dueñas-Gonzalez A. The multitargeted drug ivermectin: from an antiparasitic agent to a repositioned cancer drug. Am J Cancer Res. 2018;8(2):317-331. PubMed
- Juarez M, Schcolnik-Cabrera A, Dominguez-Gomez G, et al. Antitumor effects of ivermectin at clinically feasible concentrations support its clinical development as a repositioned cancer drug. Cancer Chemother Pharmacol. 2020;85(6):1063-1077. PubMed
- Liu J, Zhang K, Cheng L, Zhu H, Xu T. Progress in Understanding the Molecular Mechanisms Underlying the Antitumour Effects of Ivermectin. Drug Des Devel Ther. 2020;14:285-296. PubMed
- Pouliot JF, L’Heureux F, Liu Z, Prichard RK, Georges E. Reversal of P-glycoprotein-associated multidrug resistance by ivermectin. Biochem Pharmacol. 1997;53(1):17-25. PubMed